In 1959, Dr. Mildred Stahlman set out to establish the first intensive care unit for newborns at the Vanderbilt University Hospital. The unit quickly became a referral center for high-risk newborns across Tennessee and extending into Southern Kentucky and Northern Alabama. With the realization that optimal neonatal care begins in the womb, a strong bond was forged with Vanderbilt Maternal Fetal Medicine and Pediatric Surgical subspecialists, and one of the first collaborative fetal centers for diagnosis and therapy—the Junior League Center for Advanced Maternal Fetal Care—was established at Vanderbilt to facilitate coordinated diagnosis, consultation, planning and delivery of newborns with complex medical and surgical problems. We continue to follow Dr. Stahlman’s mission to foster knowledge through research, teaching and training through patient care, and a commitment to continuous improvement to delivering superb clinical care, with the overarching goal of improving the health of prematurely born infants and infants born at term with complex problems. As the Regional Perinatal Center for Middle Tennessee, we and our obstetric colleagues work with the Tennessee Department of Health to promote access to care and outreach education to reduce preterm birth, maternal mortality, and infant mortality. Our faculty's professional interests span across multiple areas:
|
|
We continue to pursue Dr. Stahlman’s passion for investigation. One of the first infant respirators was created here at Vanderbilt, and our faculty continue to strive to develop new and innovative approaches to the diagnosis, prevention and management of complications of preterm birth. From understanding the molecular changes that lead to preterm birth, to investigating the mechanisms that promote the chronic lung disease that plagues prematurely born newborns—Bronchopulmonary Dysplasia, to studying clinical systems that ensure every patient the full benefit of evidence-based practices locally and state-wide: our faculty, staff, and students are committed to fundamental and clinical discovery to benefit our patients and their families.
Education and training are integral to all aspects of our mission. This includes clinical training for residents and medical students in the Stahlman Neonatal Intensive Care Unit and the Monroe Carell Jr. Children’s Hospital NICU. We are blessed to have philanthropic support to promote the research training and academic career development for fellows through the Hooper Family Fellowship in Neonatology. In addition to funding from the National Institutes of Health, our faculty and trainees have obtained competitive grant funding from the March of Dimes, the American Heart Association, the Parker B. Francis Family Foundation, the Thrasher Foundation, and the Gerber Foundation, to name but a few of the private foundations that support our research mission. Fellows, residents, junior physician scientists and junior PhD scientists in the division have competed successfully for postdoctoral training grants (NIH R38, T32) at VUMC, and individual training grants and career development NIH awards (K12, KL2, K08, K23).
Our trainees and faculty alumni have achieved prominence as leaders in Neonatal-Perinatal Medicine as division directors, department chairs, research directors, independent scientists, and academic clinicians.
I welcome you to learn more about the division through our website and to contact us regarding opportunities for education, training and collaborations.
Best regards,

Susan H. Guttentag, MD
Director, Mildred Stahlman Division of Neonatology
Julia Carell Stadler Chair in Neonatology
Professor of Pediatrics
Vanderbilt University Medical Center
-
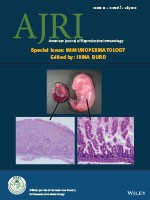
Erin M. Fricke, Timothy G. Elgin, Huiyu Gong, Jeff Reese, Katherine N. Gibson-Corely, Robert M. Weiss, Kathy Zimmerman, Noelle C. Bowdler, Karen M. Kalantera, David A. Mills, Mark A. Underwood, Steven J. McElroy. LPS‐induced maternal inflammation induces direct placental injury without alteration in placental blood flow and induces a secondary fetal intestinal injury that persists into adulthood. American Journal of Reproductive Immunology, April 2018.

Jennifer M.S. Sucre, Gail H. Deutsch, Christopher S. Jetter, Namasivayam Ambalavanan, John T. Benjamin, Linda A. Gleaves, Bryan A. Millis, Lisa R. Young, Timothy S. Blackwell, Jonathan A. Kropski, Susan H. Guttentag. A Shared Pattern of Beta-catenin Activation in Bronchopulmonary Dysplasia and Idiopathic Pulmonary Fibrosis. American Journal of Pathology, April 2018.
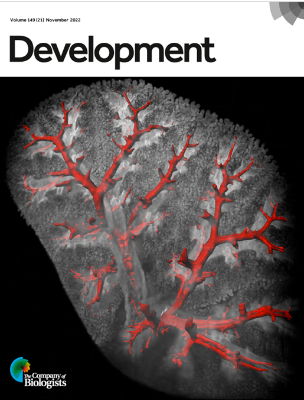
Prashant Chandrasekaran, Nicholas M. Negretti, Aravind Sivakumar, Derek C. Liberti, Hongbo Wen, Maureen Peers de Nieuwburgh, Joanna Y. Wang, Nigel S. Michki, Fatima N. Chaudhry, Sukhmani Kaur, MinQi Lu, Annabelle Jin, Jarod A. Zepp, Lisa R. Young, Jennifer M.S. Sucre, David B. Frank. CXCL12 defines lung endothelial heterogeneity and promotes distal vascular growth. Development, Nov. 2022.
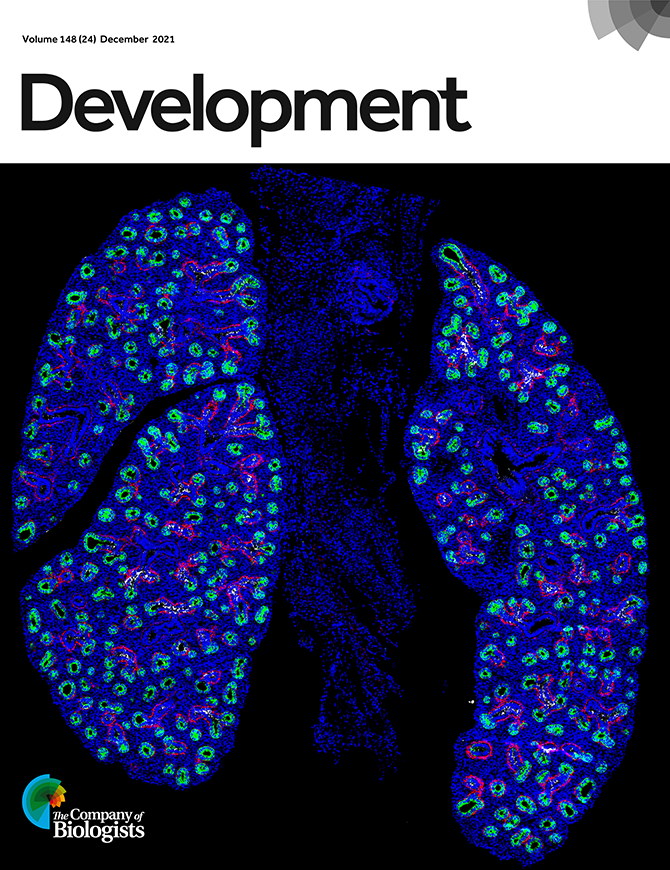
Christopher S. Jetter, Peter Gulleman, Claire Bunn, Alice N. Hackett, Meaghan Ransom, Chase J. Taylor, David Nichols, Brittany K. Matlock, Susan H. Guttentag, Timothy S. Blackwell, Nicholas E. Banovich, Jonathan A. Kropski, Jennifer M. S. Sucre. A single-cell atlas of mouse lung development. Development, Dec. 2021.
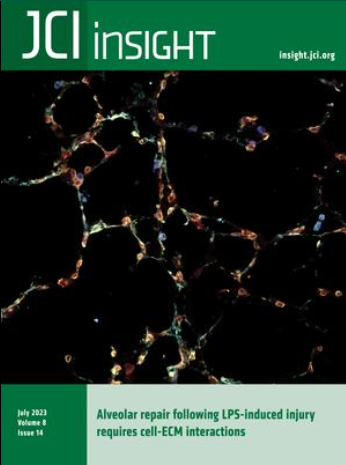
Jennifer M.S. Sucre, Fabian Bock, Nicholas M. Negretti, John T. Benjamin, Peter M. Gulleman, Xinyu Dong, Kimberly T. Ferguson, Christopher S. Jetter, Wei Han, Yang Liu, Seunghyi Kook, Jason J. Gokey, Susan H. Guttentag, Jonathan A. Kropski, Timothy S. Blackwell, Roy Zent, Erin J. Plosa. Alveolar repair following LPS-induced injury requires cell-ECM interactions. JCI Insight, June 2023.
Nicholas M Negretti, Yeongseo Son, Philip Crooke, Erin J Plosa, John T Benjamin, Christopher S Jetter, Claire Bunn, Nicholas Mignemi, John Marini, Alice N Hackett, Meaghan Ransom, Shriya Garg, David Nichols, Susan H Guttentag, Heather H Pua, Timothy S Blackwell, William Zacharias, David B Frank, John A Kozub, Anita Mahadevan-Jansen, Evan Krystofiak, Jonathan A Kropski, Christopher Ve Wright, Bryan Millis, Jennifer Sucre. Epithelial outgrowth through mesenchymal rings drives lung alveologenesis. JCI Insight, Feb. 2025.

Ashley L Mutchler, Jianyong Zhong, Hai-Chun Yang, Shilin Zhao, Rachelle Crescenzi, Shannon Taylor, Roy L Rao, Elaine L Shelton, Annet Kirabo, Valentina Kon. ET-3/ETBR Mediates Na+-Activated Immune Signaling and Kidney Lymphatic Dynamics. Circulation Research, Jan. 2025
